Cowper’s Cut 375: Wake the dead
First came Health But Social Care Secretary Wes Streeting’s official announcement on taking office last year that “the NHS is broken”.
Now we have NHS England’s chief taxidermist Sir James Mackey announcing this week that bad care has been normalised in the English NHS: “ten years ago, we would have never accepted old ladies being on corridors next to an (emergency) department for hours on end and they have become normal in the NHS. We’ve got to get ourselves out of that, and everybody wants to get out of it.”
Speaking to the Medical Journalists Association this week, Sir James expressed concern that staff had become “desensitised” to unsafe care, comparing it to “learning to walk with a limp”.
It’s been treated as news, which is odd. These are statements of the obvious, if you read the data from the latest health questions from the British Social Attitudes survey. Only one person in five (21%) of those surveyed in 2024 said they were satisfied with the way the NHS runs. Six in 10 people (59%) said they were ‘very’ or ‘quite’ dissatisfied with the NHS in 2024: up from 52% in 2023.
This is the highest level of reported dissatisfaction with the health service since the BSA survey began in 1983.
The key question remains: what clear and deliverable plans do our national leaders have to do something about this lousy state of things?
I remain unclear that there is currently a good answer available. Once again: the ‘triple shift’ (hospital to community; treatment to prevention; George to Ringo) is not a plan, but a broad ambition.
The 2025 NHS Cultural Revolution
You might be well-advised to take care with analogies linked to the Cultural Revolution, but Sir James told the gathering that NHS managers are having to be “re-educated” after losing skills in recent years, particularly in areas like waiting list management and hospital patient flow.
“We are having to re-skill [and] train people again in things like waiting list management, some stuff on flow and ED management, those sorts of things. So, they are being rebuilt, and people are being re-coached and re-educated”.
This is a fair description of the loss of management capacity and capability in many organisations, as described unsparingly in the 2024 Darzi Review.
But it raises questions: why did these skills atrophy? When did lost management skills start becoming a major problem? Was it during the time of NHS Improvement, which Sir James headed? Surely a body with such a name should have noticed, and indeed mentioned such a thing.
Money troubles
Sir James was also combative on the topic of money, saying that “the NHS is such a big part of public spending now we are pretty much maxed out on what’s affordable. It is really now about delivering better value for money, getting more change, getting back to reasonable productivity levels, but in a way that’s human and is about standards and about quality.”
While hoping for “some growth” fiscally from the Treasury in the summer’s comprehensive spending review, Mackey acknowledged that “it’s never enough”, adding that the service faces “big choices” to tackle variation and improve quality standards.
Sir James’ argument here seems tautological. If the English NHS is indeed “pretty much maxed out on what’s affordable”, then how can any token CSR growth (which is likely to be lost on wage claims) be “never enough”?
Politics as unusual

Sir James was also keen to promote NHS independence from politicians, saying “I’ll have no problem telling anybody what I think — if I have a view, I’m going to express it, and if I think something’s wrong, I’m going to say it.
Mackey added that Mr Streeting was “actually very good at being able to cope with contrary views and argument and discussion”.
This sits slightly uneasily with his subsequent comments on the ending of NHSE’s independence, that “I think it was probably, in hindsight, a bit naive to think that we could make something politically independent and less directly controlled by the political system for something that is the biggest consumer of public resource in the country”.
Sir James suggested that ministers “need control” of the NHS’s budget because they are “democratically accountable” for its spending.
Ahem. The NHS is not the ‘biggest consumer of public resource in the country’: social security is.
More to the point, Sir James has not been selected as the interim national leader of the English NHS because Team Streeting think they will disagree with him a lot.
As to the wisdom or otherwise of having an independent NHS England, one can read its travails over the past few years as telling us that what NHS England could not (and did not) survive is poor-quality and politically naïve leadership.
‘You’re fired! … oh’

The impression that the abolition of NHS England was mainly driven by Wes’ whim of the week didn’t get any weaker with the written PQs on NHS management redundancy costs and plans by Lib Dem health lead Helen Morgan, and the answers by NHS reform minister Karin Smyth.
The reply reads, “the PM announced the integration of the Department and NHS England and the associated reduction in size, and NHS England has also set out separate ambitions of reducing integrated care board running costs as well as National Health Service trusts’ corporate costs ...
“Clearly these reforms will have workforce implications, and we are working closely with NHS England and HM Treasury to deliver these, however we do not yet have a robust estimate of costs for 2025/26.
“Discussions have been with NHS England at a national level, and not with individual integrated care boards or trusts”.
Spotting a good story in the absence of an impact assessment, Morgan promptly brought this to the attention of The Guardian’s Denis Campbell.
Providing for the financial reset
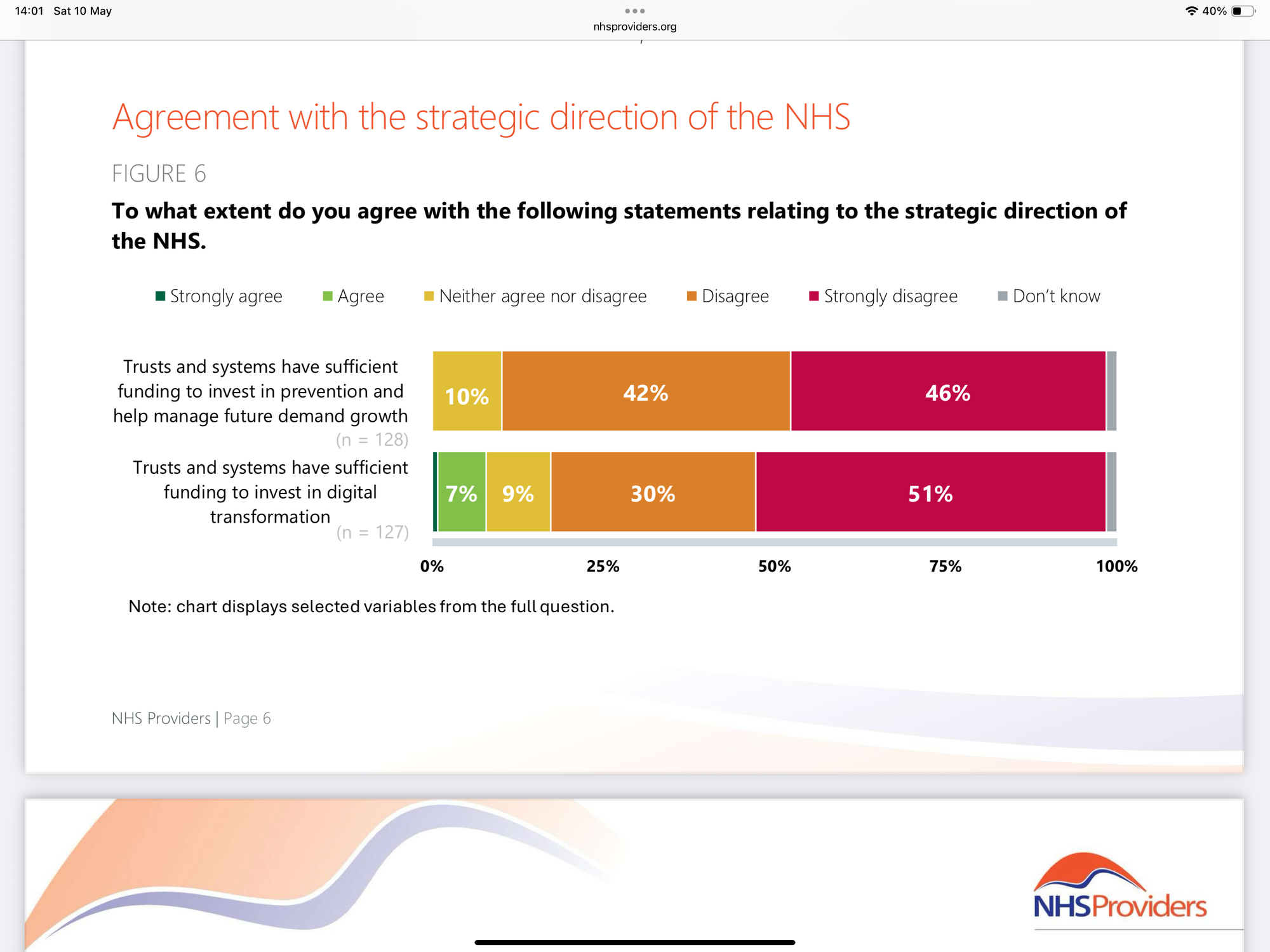
NHS Providers’ recent survey of its members on the financial reset plans described by Sir James Mackey found that:
Nearly half (47%) of those surveyed told us that they will have to scale back service provision to deliver their financial plan, and a further 43% have this currently under consideration.
More than a quarter (26%) said they will need to close some services to deliver their financial plan, and a further 55% have this currently under consideration.
Over a third (37%) of respondents said their organisation will cut substantive clinical posts to deliver their financial plan, with a further 40% saying this is currently under consideration.
Only 12% of respondents were confident they have sufficient access to capital to deliver a positive environment for staff, patients and service users. Close to three in five respondents said patient experience (61%), work to address health inequalities (60%) and access to timely care (57%) were most at risk of being impacted in order to deliver financial plans.
Nearly nine in ten (88%) respondents disagreed that trusts and systems have sufficient funding to invest in prevention and help manage future demand growth.
Eight in ten (81%) surveyed disagreed that trusts and systems have sufficient funding to invest in digital transformation.
Mmmmmmmm.
If I were Mr Wes Streeting, then I would be concerned that 88% of respondents disagreed that “trusts and systems have sufficient funding to invest in prevention and help manage future demand growth”.
It’s almost as if they don’t believe in the triple shift, which as J M Barrie and The Jackson Sisters show us, is a risky thing.
The ghosts of Mid-Staffs
Hopefully, Sir James Mackey doesn’t need telling that in all such political communications as those of the NHS financial reset, you need to be aware that what your audience hears may not be what you think you’ve told them.
This financial reset presents big, real and serious risks.
Twelve years ago, a wise man wrote of his report on a huge NHS scandal, “the story it tells is first and foremost of appalling suffering of many patients. This was primarily caused by a serious failure on the part of a provider Trust Board.
“It did not listen sufficiently to its patients and staff or ensure the correction of deficiencies brought to the Trust’s attention. Above all, it failed to tackle an insidious negative culture involving a tolerance of poor standards and a disengagement from managerial and leadership responsibilities.
“This failure was in part the consequence of allowing a focus on reaching national access targets, achieving financial balance and seeking foundation trust status to be at the cost of delivering acceptable standards of care.
“The story would be bad enough if it ended there, but it did not. The NHS system includes many checks and balances which should have prevented serious systemic failure of this sort. There were and are a plethora of agencies, scrutiny groups, commissioners, regulators and professional bodies, all of whom might have been expected by patients and the public to detect and do something effective to remedy non-compliance with acceptable standards of care.
“For years that did not occur, and even after the start of the Healthcare Commission investigation, conducted because of the realisation that there was serious cause for concern, patients were, in my view, left at risk with inadequate intervention until after the completion of that investigation a year later.
“In short, a system which ought to have picked up and dealt with a deficiency of this scale failed in its primary duty to protect patients and maintain confidence in the healthcare system.
“The report has identified numerous warning signs which cumulatively, or in some cases singly, could and should have alerted the system to the problems developing at the Trust.”
The resonance of unlearned lessons should haunt national leaders.

I wonder whether it does.
Recommended and required reading
‘Adult Social Care Reform: the cost of inaction’: the new report from the Commons Health But Social Care Select Committee.
The Treasury Munchkins’ evidence to the above inquiry.
DHBSC announcements on the ‘Cancer 360’ software rollout and extra capital funding for GP practices.
The FT reports that loss-making Xellia Pharmaceuticals, Europe’s last manufacturer of ingredients for some vital antibiotics, is closing its biggest domestic factory and shifting some production to China.
It’s five years since this HSJ-era ‘Cowper’s Cut’ said “A-haa!” to a Health Secretary with an unshakeable commitment to statistical accuracy. [Coughs]

